Pediatric Medical Imaging and Hematologic Cancer Risk: NEJM Study
NEJM study of 3.7 million children: cumulative bone-marrow radiation dose is linked to a small but significant increase in hematologic cancer risk.
Key takeaway: Exposure ≥30 mGy was associated with a 1.76× higher risk; about 10.1% of cases could be attributable to higher-dose imaging (e.g., CT). (1 head CT ≈ 13.7 mGy)
📊 Cohort & Follow-up
3,724,623 children; 35.7M person-years (mean 10.1y).
🧪 Outcomes
2961 hematologic cancers: 79.3% lymphoid, 15.5% myeloid/acute leukemia, 4.4% histiocytic/dendritic.
📈 Excess Incidence
Among ≥30 mGy (mean 57 mGy), excess by age 21 ≈ 25.6 per 10,000.
% Attributable
10.1% (95% CI 5.8–14.2) attributable to imaging-related radiation.
📏 Dose Guide (mGy)
- Chest X-ray: ~0.1 mGy (ionizing)
- Head CT: ~13.7 mGy (ionizing)
- Abdominal CT: ~15–20 mGy (ionizing)
- Ultrasound & MRI: No ionizing radiation
Remember: Risk relates to cumulative dose — repeated CTs add up.
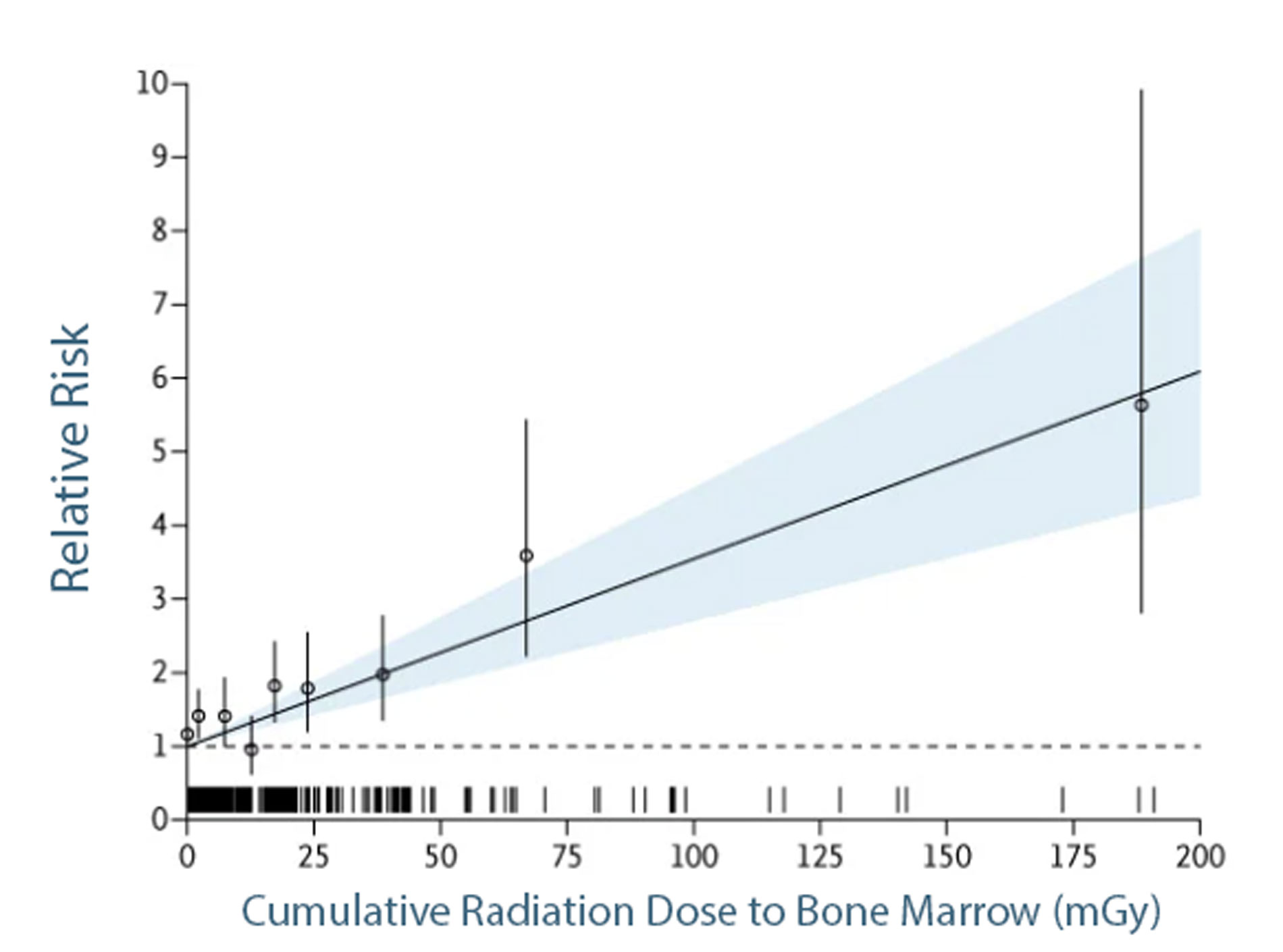
📈 Dose–Risk Relationship
⚡ Uses Ionizing Radiation
- X-ray
- CT (Computed Tomography)
- Nuclear medicine (e.g., PET, scintigraphy)
🛡️ No Ionizing Radiation
- Ultrasound
- MRI (Magnetic Resonance Imaging)
🎯 Practical Actions (ALARA)
- Justify each CT: will it change management?
- Optimize pediatric protocols; avoid repeats; size-based settings.
- Prefer US/MRI when clinically adequate.
- Track cumulative dose; communicate risks to families clearly.
📋 Relative Risk by Dose Band
| Cumulative Dose (mGy) | RR vs 0 mGy | 95% CI |
|---|---|---|
| 1–<5 | 1.41 | 1.11–1.78 |
| 15–<20 | 1.82 | 1.33–2.43 |
| 50–<100 | 3.59 | 2.22–5.44 |
| Per 100 mGy: ERR ≈ 2.54 (95% CI 1.70–3.51). 30 vs 0 mGy: RR ≈ 1.76 (95% CI 1.51–2.05). | ||
Source
Smith-Bindman R, Alber SA, Kwan ML, et al. Medical Imaging and Pediatric and Adolescent Hematologic Cancer Risk. NEJM, Sept 17, 2025. DOI: 10.1056/NEJMoa2502098